Samuel Edusa MD
Monkeypox
Samuel Edusa | Jun 3, 2022
Monkeypox has been in the news a lot recently. The virus has been present in Central and West Africa since the early 1970s, but in May 2022 it started spreading beyond that region. As of May 26, 2022, over 300 cases have been confirmed across 20 non-African countries and six US states. The situation is changing quickly.
Background
Monkeypox is an orthopoxvirus that looks clinically similar to smallpox. It was first identified in monkeys in 1958, and the first human outbreak occurred in the Democratic Republic of Congo (DRC) in the early 1970s.
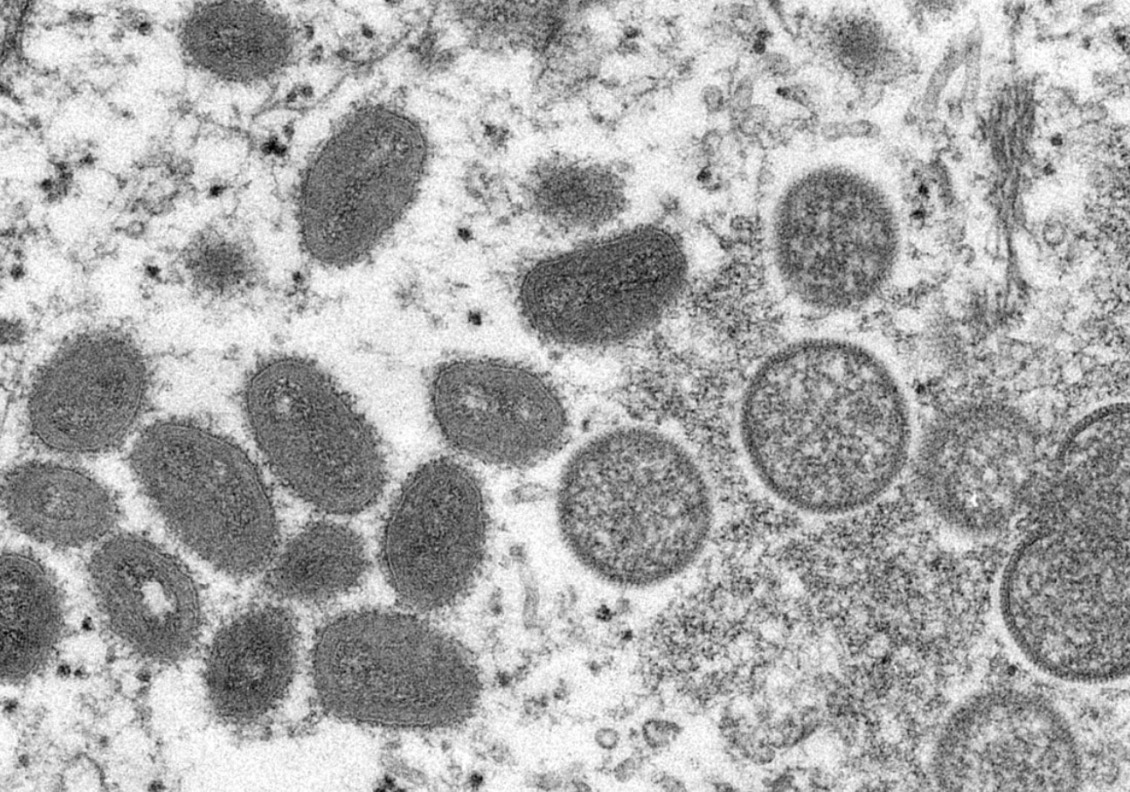 (Image from the CDC Cynthia S Goldsmith, Russell Regnery. [Public domain])
(Image from the CDC Cynthia S Goldsmith, Russell Regnery. [Public domain])
The electron microscope image above shows monkeypox virion recovered from a human skin sample during the 2003 US epidemic. Mature, oval-shaped viral particles are on the left; immature, spherical particles are on the right.
Transmission
Monkeypox is zoonotic, meaning it spreads from animals to humans, usually through contact with or consumption of small animals, especially rodents. During the 2003 US outbreak, several dozen cases were traced back to pet prairie dogs and, ultimately, rats imported from Ghana. Human-to-human transmission occurs through damaged skin, respiratory droplets, or mucous membrane contact. Indirect transmission through contaminated clothing or linens is also possible.
Several cases in the 2022 outbreak have been in men who have sex with men, which has raised questions about specific transmission pathways. However, the virus still spreads primarily through bodily fluids, respiratory droplets, and direct contact with lesions.
Signs and symptoms
Early signs include fever and lymphadenopathy (swollen lymph nodes), often accompanied by headache, muscle pain, chills, fatigue, and cough. The lymphadenopathy, particularly in the submental, submandibular, cervical, and inguinal nodes, is the most reliable feature that distinguishes monkeypox from smallpox and chickenpox.
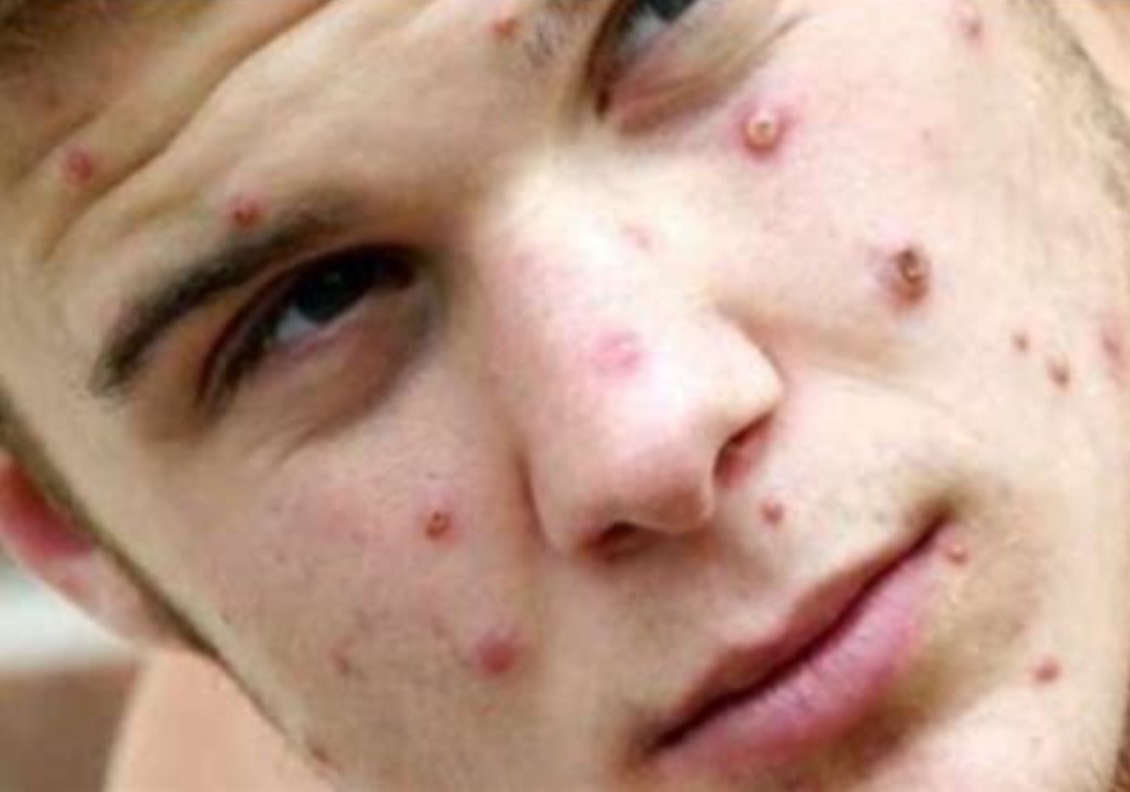 Caucasian male with monkey pox pustules on his face (Source: nairobitimes.co.ke)
Caucasian male with monkey pox pustules on his face (Source: nairobitimes.co.ke)
Incubation takes 7-14 days (range: 5-21 days). The rash appears 1-3 days after fever onset, typically starting on the face and mouth before spreading to the rest of the body, including palms and soles. It looks like chickenpox. Lesions progress through macular, papular, vesicular, and pustular stages before resolving. The illness lasts 2-4 weeks, with ulcerative lesions in some cases.
Evaluation
Use droplet precautions when examining a suspected case: N95 mask, gown, gloves, and eye protection. Get a thorough travel and exposure history. Track all clinical staff who had contact with the patient. Disinfect room surfaces after the patient leaves.
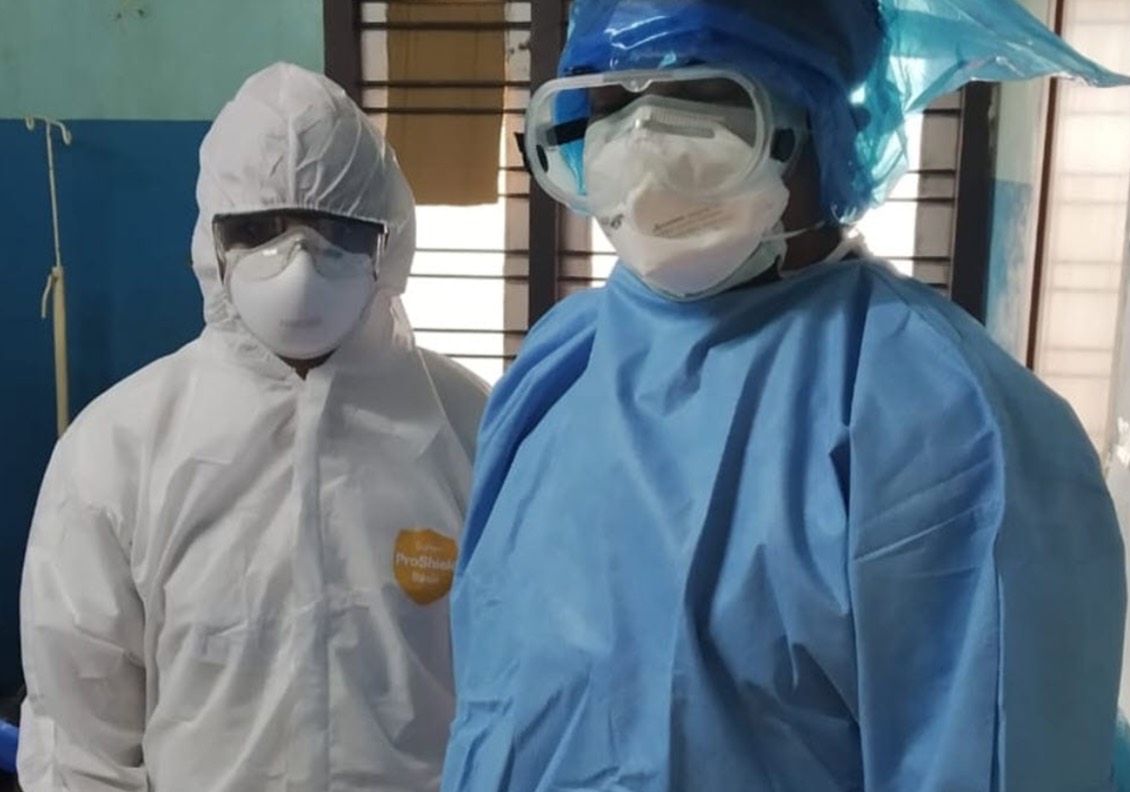 Image of clinicians wearing personal protective equipment (PPE) from Wikimedia Commons | Javed Anees, District Hospital, Tirur.
Image of clinicians wearing personal protective equipment (PPE) from Wikimedia Commons | Javed Anees, District Hospital, Tirur.
Collect viral cultures via oropharyngeal or nasopharyngeal swab. Skin biopsy of a vesiculopustular lesion or fluid from an intact vesiculopustule should also be examined. Confirmation can be done with PCR, electron microscopy (if other orthopoxviruses are excluded), or immunohistochemistry. A Tzanck smear can help rule out nonviral causes in the differential, but it can't distinguish monkeypox from smallpox or herpes.
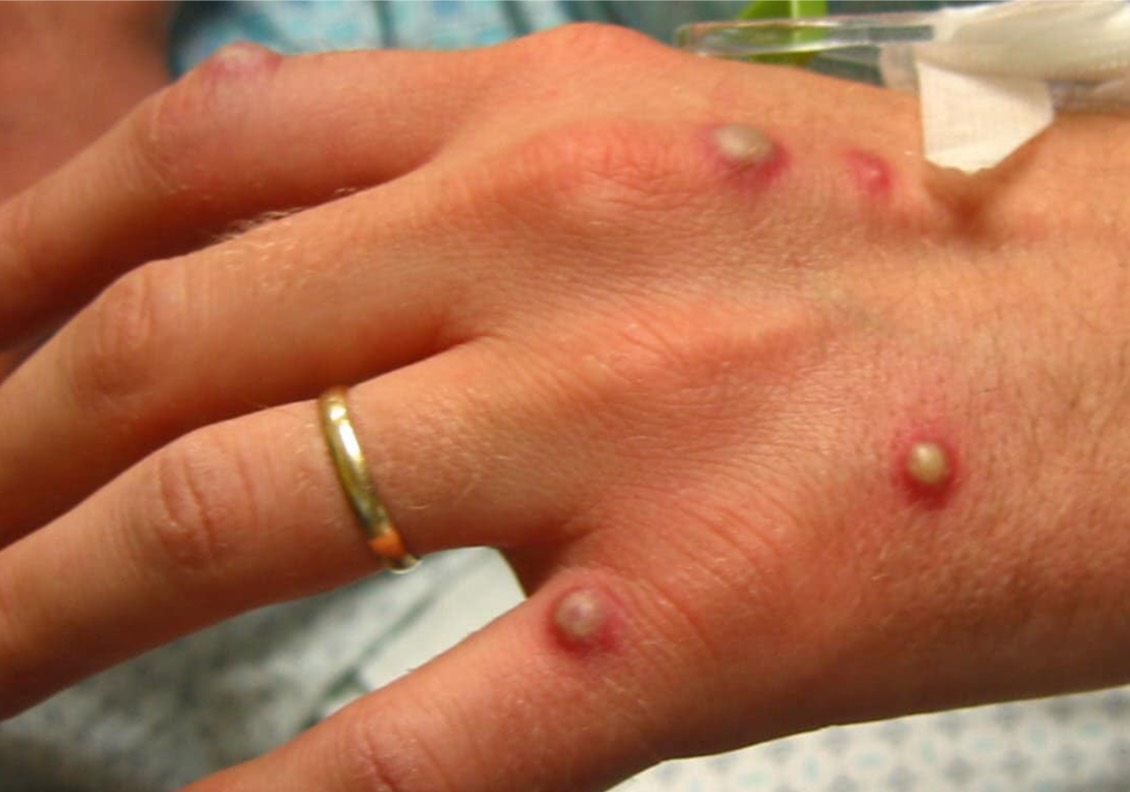 Image courtesy of Medscape. The dorsum of a patient's hand has a monkeypox vesiculopustular rash. Some lesions have a central umbilication.
Image courtesy of Medscape. The dorsum of a patient's hand has a monkeypox vesiculopustular rash. Some lesions have a central umbilication.
Treatment
Treatment is mostly supportive and symptomatic. Isolate the patient and use appropriate precautions. The patient remains infectious until all scabs have dried and fallen off. Vaccines are available, and post-exposure vaccination after high-risk contact has been shown to prevent or reduce severity of illness.
Mortality and complications
Mortality rates in Africa range from 1.0% to 10.6%, with immunocompromised and malnourished patients at highest risk. Secondary bacterial infections can develop from the skin lesions.
